Virological assessment of fetuses and neonates
exp date isn't null, but text field is
| West of Scotland SPECIALIST VIROLOGY CENTRE Level 5 New Lister Building, Glasgow Royal Infirmary, 10-16 Alexandra Parade, Glasgow, G31 2ER |
- Contacting Laboratory - email rather than phone: west.ssvc2@nhs.scot
- Opening hours - weekdays 8am-8pm; weekends 8am-6pm
Out of hours - contact on call medical virologist via GRI switchboard ( 0141 211 4000 )
- There are only a limited number of tests available out of hours.
- Routine samples are delivered to the laboratory by porter/ pod system/ via other labs.
- For urgent samples during working hours phone the lab and arrange a taxi. Check when the results are likely to be available and provide us with contact details.
- All authorised results are available via SCI store or clinical portal providing the CHI number is included on the request form.
- Swabs should be placed in VPSS. VPSS has a long shelf life at room temperature and is suitable for all types of swab including eye swabs (chlamydia). Use a dry swab, squeeze the swabbed material into VPSS or VTM by pressing against the side of the vial and discard the swab. Do not leave the swab in the medium. VPSS is an irritant and should not come into contact with the baby
- VPSS can be obtained directly from us or via local microbiology service.
- Always provide clinical details including age, gestation, date of onset of symptoms and any fetal abnormalities (if relevant). This helps with test selection.
- We no longer perform TORCH screens or test babies with a diagnosis of conjugated hyperbilirubinaemia. Phone the lab to discuss.
- It is helpful to provide the mother’s name and date of birth. Testing of antenatal samples may help confirm or rule out a specific infection.
- Routine testing of maternal or fetal samples from IUD cases is rarely helpful. If a specific pathogen is suspected please write this on the form and send with a small piece of placental tissue (not swab).
- Amniotic fluid / fetal blood samples can be tested but not until at least 6 weeks post acute illness, and not before 18-20 weeks gestation.
- As a general principle always take a sample from the affected system.
- Classical features of in utero infections include the following:
CMV Hepatosplenomegaly, microcephaly, chorioretinitis, cerebral calcification, thrombocytopaenia. (see WoS guideline for management) Rubella Cardiac, ocular and neurological defects, hepatosplenomegaly, purpura. This is extremely rare. Toxoplasma Hydrocephalus, retinochoroiditis, hepatitis, pneumonia, myocarditis Erythrovirus B19 Fetal anaemia / hydrops
(B19 is not associated with congenital malformation) - Congenital CMV is diagnosed by sending a urine +/- saliva for CMV PCR testing. This must be done within 21 days of life
- To diagnose HIV infection, see WoS policy or discuss with virology.
- Testing for HBV or HCV in the under 1’s is not recommended as maternal antibodies may still be present. Please discuss with virologist if testing is required.
- If HSV disease is suspected send swabs, urine and blood +/- CSF. Surface swabs and a blood are required if the baby has been exposed but is not showing signs of infection. (see WoS guideline)
- Diagnosis relies on samples taken from the system(s) involved (see table).
- Most tests use PCR technology, these take an average 3-5 hours to complete from arrival in the lab. Most of the tests are multiplexed. This means that a sample may be tested for more viruses than you requested
|
Respiratory Screen by PCR (2 parts) In addition, CMV is tested on the respiratory secretions of all babies <21 days of age & Chlamydia is tested on all negative samples in babies (<2month age). |
| Blood – CMV, EBV, adenovirus, HSV |
| CSF – HSV1/2, VZV, enterovirus. |
| Skin swab – HSV/VZV. |
| Stool samples – norovirus, rotavirus, sapovirus, astrovirus, adenovirus |
| Eyes – HSV, VZV, Adenovirus, Chlamydia trachomatis |
- In situations which have infection control implications (e.g. outbreak or VZ contact), please contact the lab and infection control to coordinate testing.
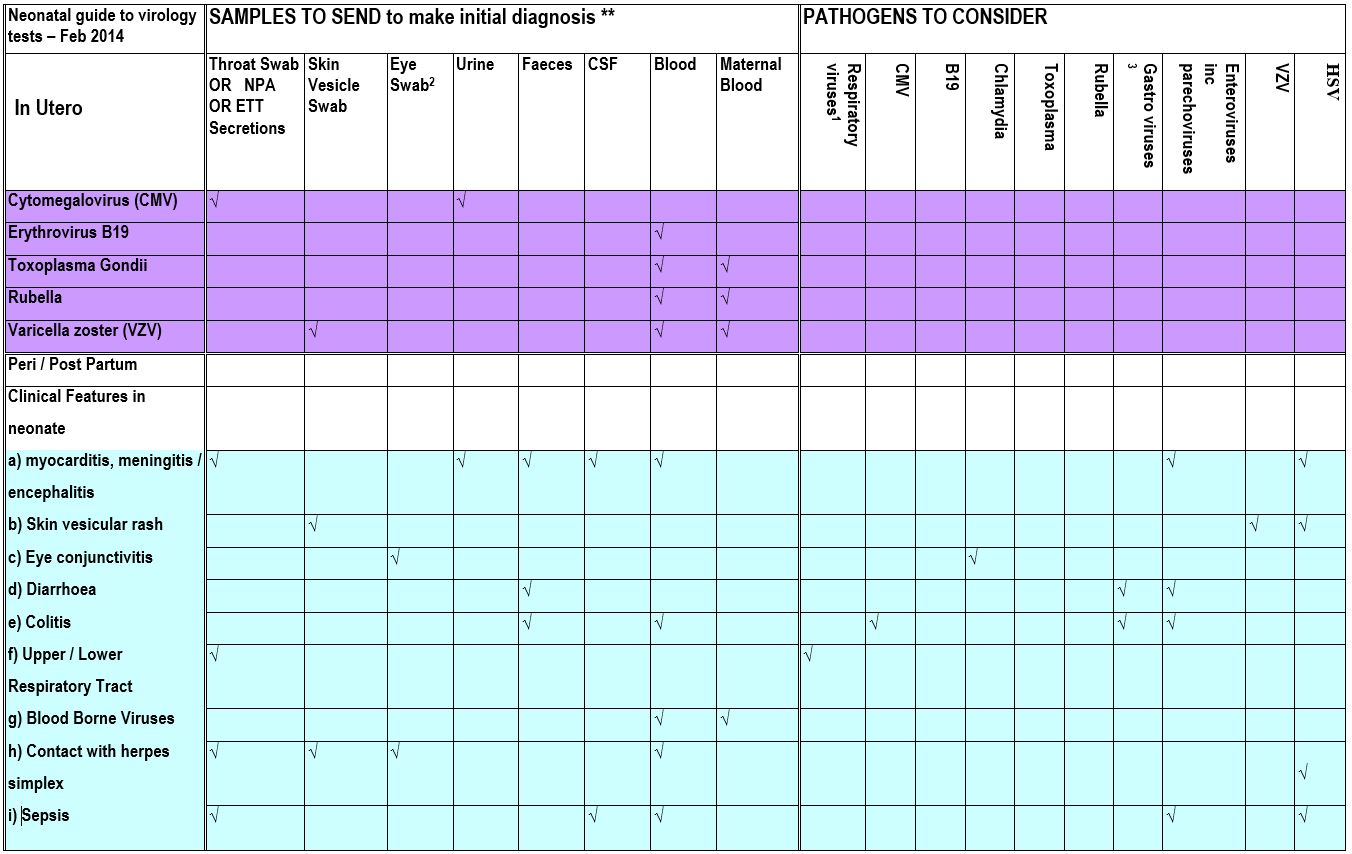 ** Samples are from the neonate unless otherwise specified
** Samples are from the neonate unless otherwise specified
Last reviewed: 01 August 2021
Next review: 01 August 2024
Author(s): Dr C Aiken, Consultant Virologist
Approved By: MCN for Neonatology, West of Scotland
Reviewer Name(s): Dr Celia Jackson, Consultant Virologist

